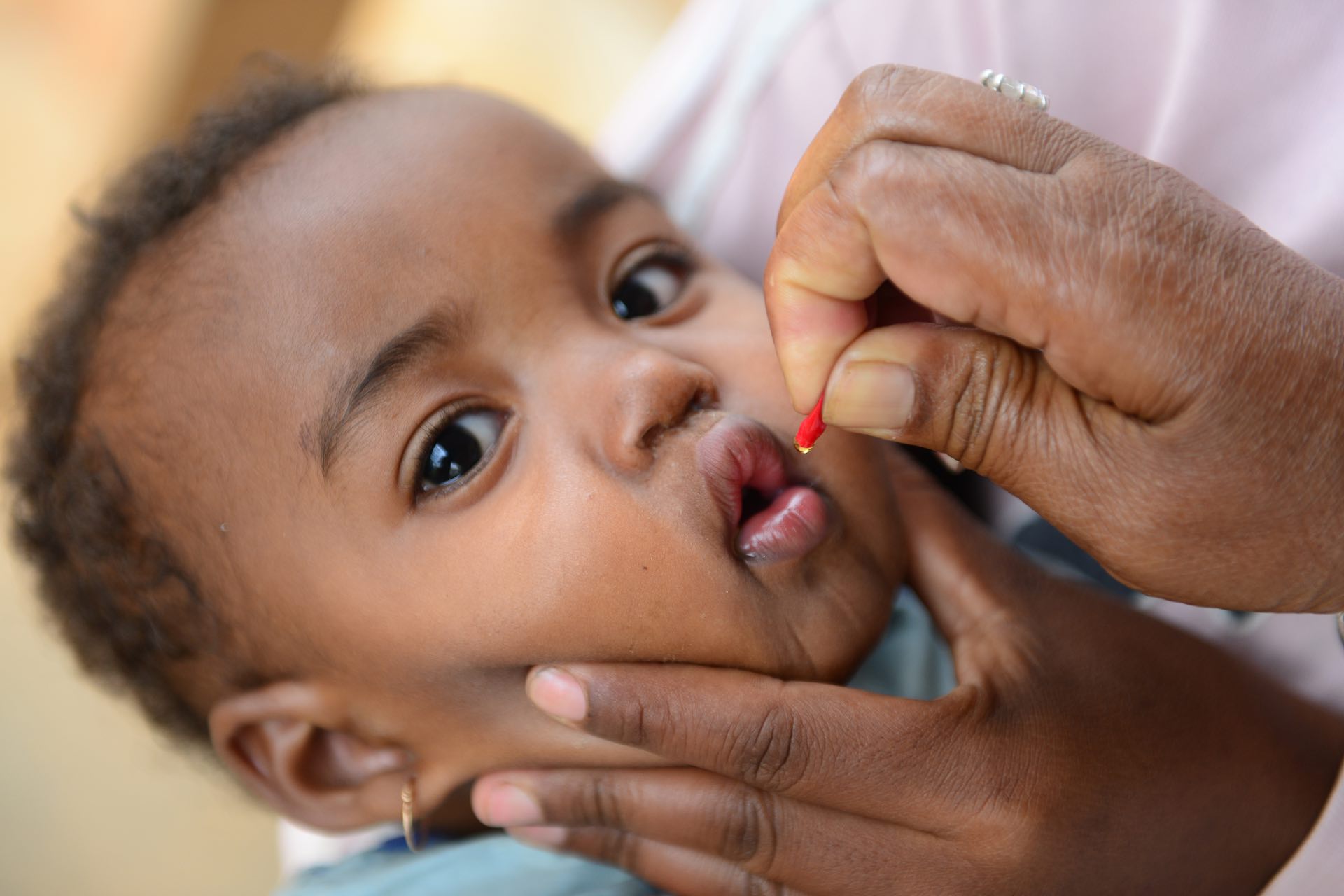
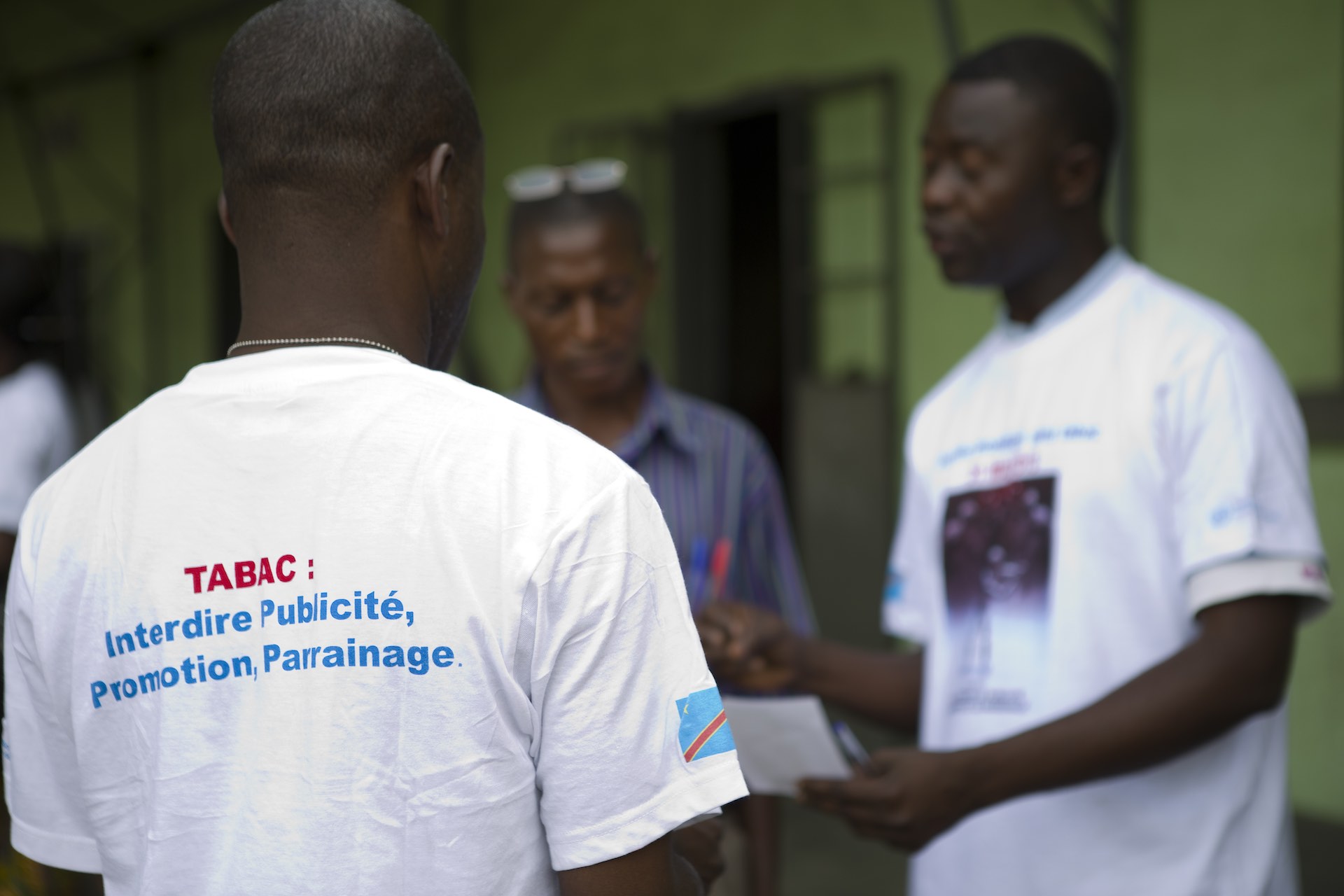The Healthier Populations (UHP) Cluster in the African Region is designed to support Pillar 3 of WHO’s 13th Global Programme of Work (GPW13) which aims to make 1 billion people healthier by reducing health inequities, preventing diseases and injuries, addressing health determinants, and promoting partnerships for collaborative actions amongst all stakeholders.
Healthier Populations (UHP) Cluster
Healthier Populations (UHP) Cluster
Overview
Related health topics
Promoting health and preventing disease is a critical component of the effort required to achieve Universal Health Coverage (UHC). to date, efforts to achieve UHC have focused mostly on strengthening health systems and their capacities to provide curative care. However, experience from the COVID-19 pandemic has reaffirmed the need for resilient health systems, emphasizing primary health care, including preventive and promotive health and well-being.
Emerging from the eye of the storm as the global health lead agency during the pandemic, WHO is equipped with the required insights and actions for a holistic approach to “building back fairer and better” after COVID-19.
The Healthier Populations (UHP) Cluster in the African Region is designed to support Pillar 3 of WHO’s 13th Global Programme of Work (GPW13) which aims to make 1 billion people healthier by reducing health inequities, preventing diseases and injuries, addressing health determinants, and promoting partnerships for collaborative actions amongst all stakeholders.
Message from Dr Adelheid W. Onyango
Director, Universal Health Coverage/Healthier Populations (UHP) Cluster
Since 1948, the World Health Organization (WHO) has been leading the movement towards enhancing population health and well-being. The global average life expectancy at birth has increased from 47 years in 1950–1955 to 72 years in 2015–2020 (united nations data), an increase of 25 years or 54%.
Today, we reap its benefits from an economic perspective, having witnessed a rise in the value of health capital, which is at par with all other forms of capital combined. Investing in well-being and health lays the foundation for a prosperous and happy nation.
The COVID-19 pandemic, a combined health and economic crisis, is the most significant challenge that the world has confronted in a century. The International Monetary Fund has estimated a cumulative economic loss of US$ 22 trillion due to the pandemic.
Apart from the pandemic, issues such as climate change, biodiversity loss, pollution, rapid urbanization, geopolitical conflict and militarization, demographic change, population displacement, poverty, and widespread inequity constitute a perpetual risk of future crises that could be more severe than those experienced to date.
Preparedness requires investments integrating ecological, societal, and community and individual health and wellbeing. This calls for strengthened social structures that enable people to take control of their lives and health.
The universal Health Coverage/Healthier Populations (UHP) Cluster was established in the WHo regional office for Africa in October 2019, bringing together five technical units to implement Pillar 3 of WHo’s thirteenth Global Programme of Work (GPW13). The Cluster works across five priority areas to address determinants of health and create safe and equitable societies, reduce risk factors through multisectoral action, and create healthy settings for populations in the African region. The UHP workstreams offer entry points for the intersectoral engagement required to advance the paradigm shift toward greater emphasis on health care rather than sick care, as the Director General’s top priority in supporting countries to accelerate health.
Investing in health is the basis of an equitable, safer, and more prosperous world. The ultimate measure of our success is thriving individuals, families, communities, and nations who enjoy the highest attainable level of health and well-being.
Climate Change, Health and Environment↑
Health Promotion and Social Determinants of Health↑
Nutrition and Food Safety↑
Objective
Guide the Member States to address malnutrition and food safety, with a focus on the following:
- Implementing the Comprehensive Implementation Plan on maternal, infant, and young child nutrition to achieve six WHA targets by 2025 and end all forms of malnutrition by 2030.
- Reducing obesity and noncommunicable diseases by promoting healthy, safe, and sustainable diets and regulating food and non-alcoholic beverages.
- Integrating essential nutrition life course services through existing healthcare delivery platforms. This includes maternal nutrition interventions for women of reproductive age, and appropriate infant and young child feeding to reduce life-long risks of undernutrition and overweight, such as supporting initiatives for the prevention and management of overweight and obesity.
- Transforming food systems to provide sustainably produced safe and healthy diets, supporting countries in preventing undernutrition and treatment of acute wasting, accelerating actions on reduction of anemia, and supporting and strengthening the capacity of nutrition data systems and use.
- Reducing the burden of foodborne diseases through improved food safety systems that include up-to-date food laws, regulations, and standards.
- Increasing capacity to implement risk-based food inspection, foodborne disease surveillance, and contaminant monitoring programmes.
- Supporting implementation of food safety training programmes for food business operators in formal and informal markets; and raise consumer awareness and education programmes in communities, schools, and other settings to drive enhanced food safety practices.
- Promoting the One Health approach to address food safety concerns and reduce zoonotic diseases and antimicrobial resistance.
- Supporting the integration of nutrition and food safety actions in the Emergency Response Framework and respond to emergencies and outbreaks. Countries facing nutrition and food crises receive priority support throughout the response’s planning, implementation, and monitoring. Promoting environmentally sustainable diets while improving health has become a global priority. WHO is working with the African Union Commission and the FAO to integrate food safety in implementing the Africa Continental Free Trade Area Agreement.