Centre of excellence brings hope for sickle cell patients in Congo Republic
Brazzaville, Republic of Congo. 19 June 2019 - Worried but calm, Marcel gazes at the door of the room where his nine-year-old son, Mordecai, is receiving care. His face displays the same expression of weariness as on those of other patients and garde-malades – as family members caring for a patient are commonly called here.
He is in the waiting room of the National Reference Centre for Sickle Cell Disease (CNRD), a specialized medical centre in Brazzaville, the capital city of the Republic of Congo. Nested within Brazzaville’s main teaching hospital but enjoying management autonomy, CNRD aims to be a one-stop shop for people who, like little Mordecai, suffer from sickle cell disease.
Sickle cell disease is a major genetic ailment that affects most countries in the African region of the World Health Organization (WHO). The condition distorts the shape of the red blood cells, changing them from round to sickle-shaped which means that they can hold less oxygen and are more likely to clump together to form clots. The majority of children with the most severe form of the disease die before the age of five, usually from an infection or severe blood loss. In Congo, more than 25% of the population – about 1.4 million people - carries the gene for sickle cell.
Although his family knew that Mordecai had the disease, the frequency of the attacks increased about two years ago. His father took him to the local hospital in Talangaï, a district on the northern outskirts of Brazzaville, where Marcel lives with his wife and their three children. It was a difficult experience, Marcel recalls. “There are no specialists for sickle cell disease there. At CNRD, on the other hand, you have specialists who exclusively take care of sickle cell patients,” he says.
“When I brought the child here three days ago, I had very little money, almost nothing,” Marcel recalls. “Fortunately, Prof. Elira Dokekias was there and he took care of him right away. In fact, our first day here was entirely paid for by the centre, including prescription drugs.”
One professor’s ambition
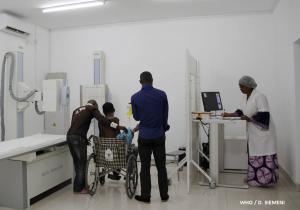
CNRD opened its doors in 2015 and treated more than 8 000 patients in its first six months of operation. The facility includes 23 beds, a blood bank, a rapid screening device, a pharmacy, an X-ray room, and a cafeteria where the menu takes the nutritional needs of sickle cell patients into account. There is also a guest house for research fellows from other countries.
“Our aim is for CNRD to serve as a regional hub,” says Professor Alexis Elira Dokekias, the centre’s director. “We want it to be a centre of excellence in research, screening, treatment and follow-up for people with sickle cell disease.”
An epidemiological survey of sickle cell disease will be carried out over the next three months, covering the whole country for the first time since 1984. Prof. Elira Dokekias also plans to set up a databank for genetic sampling and analysis, as well as a specialized curriculum and degree course on sickle cell disease for doctors and nurses. The courses will be run at the Marien Ngouabi University in Brazzaville from the 2020 academic year. He also hopes to perform perinatal screenings so as to detect signs of the disease as early as is feasible.
CNRD and the Howard University Center for Sickle Cell Disease in Washington, United States, have signed two agreements for collaboration. Together, they are currently working to develop a haematology training centre in Brazzaville. The university also helped to recruit a Congolese doctor to work at CNRD with the understanding that she will liaise on clinical care and research between the two sites.
“We hope that the Republic of Congo will be the first country in Africa to have a universal newborn screening program,” says Prof. James G. Taylor VI, the director of the Howard University centre.
“The challenges of sickle cell disease in Africa are comparable to those we face in the United States. A lack of funding and an insufficient number of trained healthcare personnel are barriers to care and research,” Prof. Taylor says.
There are reasons to be optimistic in the near future, he says. “In Africa, there have been some important political allies who have highlighted the importance of this disease,” he added.
A first lady’s advocacy
Chief among them is undoubtedly the First Lady of Congo, Antoinette Sassou Nguesso, who is also the centre’s namesake. Through Congo Assistance, her non-profit foundation, she brought sickle cell disease to the attention of the government and mobilized resources for CNRD. In May, at the 72nd World Health Assembly in Geneva, Mrs Sassou Nguesso was recognized for her commitment to the cause of sickle cell disease.
WHO provided technical expertise for the operationalization of CNRD and equipped it with an automated blood analysis device. In addition, the Organization also provided technical and financial support to strengthen the capacity of other hospitals in the country to detect and manage sickle cell disease. WHO and the Congolese Ministry of Health are planning a joint mission to further strengthen the response to sickle cell disease.
Thanks to these efforts, sickle cell patients like Mordochai can look forward to a brighter future.
Communications Officer ai
WHO Congo
Tel: +242 06 624 9763
Email: moussokij [at] who.int (moussokij[at]who[dot]int)
Technical Officer, Web & Social Media
gouahingae [at] who.int (gouahingae[at]who[dot]int)
+242 04 421 8736