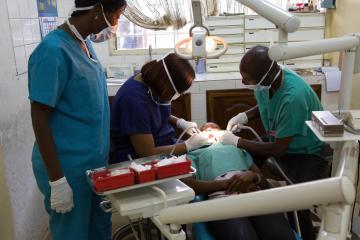
There are six conditions that make up the bulk of the oral disease burden in the WHO African Region. These are dental caries, or tooth decay; periodontal (gum) disease; oral cancers; oral manifestations of HIV infection; oro-dental/facial trauma; cleft lip and palate. Specifically in the Region, the spectrum of oral diseases also includes noma, which is a gangrenous disease that affects mainly children between the ages of 2 and 6 years. Almost all of these conditions are largely preventable or can be treated in their early stages.
Untreated dental caries/tooth decay of permanent teeth is most prevalent diseases globally and regionally, and 28.5% of the population ages greater than 5 years in the WHO African Region was estimated to be suffering from untreated caries of their permanent teeth in 2019.
In deciduous (primary) teeth, untreated caries is the single most common chronic childhood disease, 38.6% of children aged 1-9 years in the Region was estimated to be affected by untreated caries of their deciduous teeth in 2019.
Dental caries/tooth decay occur when microbial biofilm (plaque) formed on the tooth surface converts the free sugars contained in food and drinks into acids that dissolve tooth enamel and dentine over time. With continued high intake of free sugars, inadequate exposure to fluoride and without regular microbial biofilm removable, tooth structures are destroyed, resulting in development of cavities and pain, impacts on oral-health-related quality of life, and, in the advanced stage, tooth loss and systemic infection.
Periodontal (gum) disease manifests as swollen, painful, or bleeding gums and bad breath. Like dental caries/tooth decay, it is caused by poor oral hygiene, but can also be caused by smoking. In severe cases, the teeth can be detached from the gum and supporting bone and become loose. It was estimated that 22.8% of persons aged 15 years or more in the WHO African Region suffered from severe periodontal (gum) disease that may cause tooth loss in 2019.
Oral cancer includes cancers of the lip and all subsites of the oral cavity, and oropharynx. They often appear initially as a persistent ulceration, and can cause pain, swelling of the soft tissue in the mouth and throat, bleeding, or difficulty in eating or speaking.
Estimated age-standardized incidence rates of oral cancer (cancers of the lip and oral cavity) vary from low to high across countries within the WHO African Region, with a range of between 0.4 and 6.6 per 100 000 people in 2020. These differences largely follow patterns of the main risk factors for oral cancer, including tobacco use, alcohol use and Khat, and oral cancers have increased in countries with a rising prevalence of these risk factors.
Lesions in the mouth are common among people with HIV. Oral manifestations occur in 30–80% of people with HIV, with considerable variations depending on factors such as affordability of standard antiretroviral therapy (ART).
Oral manifestations include fungal, bacterial, or viral infections of which oral candidiasis is the most common and often the first symptom early in the course of the disease. Oral HIV lesions cause pain, discomfort, dry mouth, eating restrictions and are a constant source of opportunistic infection.
Early detection of HIV-related oral lesions can be used to diagnose HIV infection, monitor the disease’s progression, predict immune status, and result in timely therapeutic intervention. The treatment and management of oral HIV lesions can considerably improve oral health, quality of life and well-being.
While absence of surveillance data, oro-dental/facial trauma is a widespread yet often overlooked condition, defined as an impact injury to the teeth and/or other hard and soft tissues inside or around the mouth and oral cavity. Trauma to the teeth and face can result from a wide range of causes, including interpersonal violence, conflict, road traffic injuries, or accidents in the home, school, or workplace. Common conditions include chipped, broken, or lost teeth, dislocated jaws, and fracturing of facial bones and jawbones.
Clefts of the lip and palate are heterogeneous disorders that affect the lips and oral cavity and occur either alone (70%) or as part of a syndrome, affecting more than 1 in 1000-1500 newborns worldwide.
Although genetic predisposition is an important factor for congenital anomalies, other modifiable risk factors such as nutrition deficits and smoking during pregnancy, also play a role. This underlines the importance of antenatal care and support for pregnant women. Diagnosis and treatment of clefts present a significant challenge to public health, particularly in lower-middle income countries where availability, access and affordability of complex, multidisciplinary care are limited and complications from untreated clefts may result in high rates of infant mortality. If lip and palate clefts are properly treated by surgery, complete rehabilitation is possible.
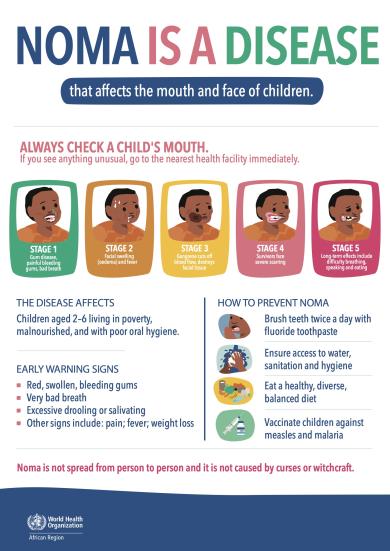
Noma is a noncommunicable gangrenous disease that affects mainly children between the ages of 2 and 6 years suffering from malnutrition, affected by infectious disease, living in extreme poverty and with weakened immune systems. Noma is mostly prevalent in sub-Saharan Africa, but sporadic cases are also reported from other world regions. Noma starts as a soft tissue lesion (a sore) of the gums, inside the mouth. The initial gum lesion then develops into an ulcerative, necrotizing gingivitis that progresses rapidly, destroying the soft tissues and further progressing to involve the hard tissues and skin of the face.
In 1998, WHO estimated that there were 140 000 new cases of noma annually. However, due to the lack of robust estimate and systematic reporting, the true global burden of noma and its distribution have been difficult to plot accurately. Without treatment, noma is fatal in 70 to 90% of cases. Where noma is detected at an early stage, its progression can be rapidly halted, through basic hygiene, antibiotics, and nutritional rehabilitation. Such early detection helps to prevent suffering, disability, and death. However, the great majority of affected communities in Africa are situated in peri-urban and rural areas where traditional beliefs and stigma are prevalent, and early detection, diagnosis and access to care are difficult. Survivors suffer from severe facial disfigurement, have difficulty speaking and eating, face social stigma, and require complex surgery and rehabilitation.