Improving emergency care for sick children
Ebie Williams brings her grandchild, Moses, to the main government hospital in Kenema. She enters the hospital barefoot, having rushed from her home, in tears. She tells how the child fell into terrifying convulsions before finally losing consciousness.
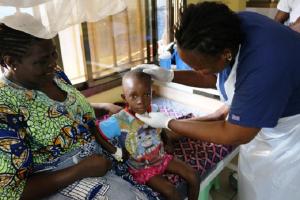
Fortunately, on this occasion, staff at the facility are able to resuscitate Moses. As soon as he arrives in the triage area the nurses quickly assess him and ensure he gets urgent treatment, which is for complications of severe malaria. This rapid treatment enables him to make a full recovery. For Ebie, her ordeal is over as she learns that the child has survived.
Sadly, there are many children who are not so fortunate. Malaria is a major cause of childhood death across Sierra Leone and very often, carers only seek treatment for their children at a late stage when complications are already severe. Pneumonia and diarrhoea are also common causes of childhood mortalities in Sierra Leone, necessitating urgent provision of oxygen or fluids to save lives.
A new programme is helping improve quality of emergency care
In addition to community engagement which promotes early treatment-seeking behaviour, efforts are also underway to strengthen the quality of emergency care for sick children.
This is why the Ministry of Health and Sanitation with support of the World Health Organization and UK aid has introduced the Emergency Triage Assessment and Treatment (ETAT+) programme in all districts, training hospital doctors, Community Health Officers, midwives and nurses to strengthen emergency paediatric care.
More than 200 health workers have so far been trained through a three-month on the job ETAT course, including 35 health workers from the Kenema Government Hospital. Necessary equipment has also been provided, with logistical support to ensure ease of access to essential drugs and supplies.
Accelerating triage and treatment time within the major hospitals
And the ETAT+ programme has already shown highly promising results. It was first piloted at the Ola During Children’s Hospital in Freetown with support from the UK’s Royal College of Paediatrics and Child Health. Not only have child survival rates there improved, nurses participating in the programme were found to be three times more likely to correctly identify children needing emergency and priority treatment, and time to treatment was reduced from three to less than one hour.
These results are in line with international evidence from other countries such as Malawi where facility-based childhood mortality almost halved in facilities where ETAT has been successfully implemented.
Putting the ETAT programme into practice
In the Kenema Government Hospital, staff say they now feel more confident in carrying out their duties. “Before now, there were too often delays in commencing care for emergency cases,” says Abibatu Sesay, a nurse at the critical care unit. “We can now do preliminary assessments and provide initial treatments for very sick children, while bringing the doctors on board as soon as possible. That is how we were able to save the life of Moses and many like him.”
As well as providing clear guidelines for triage and provision of immediate treatments for common conditions such as oxygen, fluids, antibiotics and antimalarials, the ETAT approach also helps relieve the burden on the hospitals’ limited number of medical doctors. This allows the doctors to prioritize more complex interventions, while ensuring their crucial role in the treatment process.
ETAT+ is currently being rolled out to all regional and district hospitals, with plans to expand the approach to neonatal care.