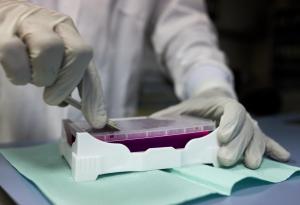
Expanding COVID-19 tests in Africa’s most populous nation
Abuja – What does it take Africa’s most populous country to curb the spread of COVID-19? When Nigeria reported its first case of the virus on 27 February 2020 it had only five laboratories in four states able to test for COVID-19. As infection spreads to more states the Nigeria Centre for Disease Control (NCDC) is ramping up testing capacity. There are now 17 laboratories and plans are afoot to set up one each in all the 36 states. Widespread testing sits at the heart of Nigeria’s COVID-19 battle.
Over the next three months, the NCDC targets to test about two million people. “To achieve this ambitious target, we have to perform 50 000 tests per state. This would require enormous investment and we are working with our partners to achieve this,” says NCDC Director-General Dr Chikwe Ihekweazu.
As measures were readied to tackle COVID-19 before the first case was detected, Nigeria, with the help of World Health Organization (WHO) and Africa Centres for Disease Control and Prevention and other partners, set up the National Reference Laboratory, in the capital Abuja, and was able to test for COVID-19 in early February. “It took a mammoth effort from NCDC, WHO and partners to buy and ship kits to Nigeria,” said Dhamari Naidoo, the focal point on laboratories at WHO Nigeria.
WHO has provided technical support, reagents and consumables as well as supporting sample transportation at the state level, and more recently in collaboration with NCDC, using virtual training to scale up capacities for sample collection. The Organization also supported the development of the national testing strategy and is working closely with all partners to implement all prongs of the strategy.
Challenges
A slowdown in global manufacturing of medical supplies against a high demand have made procurement difficult, explains Naidoo. Nigeria is currently testing 4000 samples per week.
“We are working with all partners to ensure we provide an uninterrupted supply chain to Nigeria. This includes working with private sector and very critically the UN agencies in Nigeria,” says Naidoo. “We are also exploring ways to improve efficiencies in our laboratory processes for quicker testing and testing at larger volumes. We are also working with PEPFAR (The Unites States President’s Emergency Plan For AIDS Relief) and the national TB network to integrate existing technologies and resources.”
Celestina Obiekea, a technical advisor at the NCDC, says that lack of compatible equipment was a hinderance to rapidly scale up COVID-19 testing even though the country has several molecular laboratories.
Wholesome response
A key strategy is to test, identify and isolate positive COVID-19 cases. However, increasing testing capacity must be aligned with a well-planned surveillance and contact tracing strategy as well as availability of health facilities to isolate and care for confirmed patients.
In Lagos state, the epicentre of the outbreak in Nigeria, multipartner response teams are working hard to support the state to scale up sample collection, a key requirement to enable increased testing. A decentralized approach at local government area (an administrative unit) level allows easier sample collection at the community level.
This expansion requires additional resources such as more investigation teams, vehicles and resources for sample collection and personal protective equipment. Teams need to move from house to house working long hours every day searching people who may have contracted the virus. Samples are collected from people who meet the criteria for testing and the sample is then transported to the distribution point at the Lagos State Biobank laboratory.
Dr Babatunde Saka of the State Biobank laboratory says that the efficiency of the laboratory relies on adequate manpower, good surveillance and well-designed sample collection and logistics plan.
Increased testing also requires that hospitals have the right capacity to isolate and care for patients to avoid overwhelming an already fragile health system. Lagos state is currently increasing the number of hospitals available by re-modelling existing facilities and building additional facilities.
Dr Otim Patrick Ramadan, an epidemiologist with WHO, is working with a team to enhance surveillance in communities and in health facilities.
“Access to testing capacity is quite essential for the control of a highly transmissible disease like COVID-19 so that suspected cases identified in the community are quickly tested and once confirmed rapidly isolated to curb further transmission,” he says.
Communications Officer
WHO Nigeria
Email: hammanyerok [at] who.int (hammanyerok[at]who[dot]int)
WHO Regional Office for Africa
Acting Regional Communications Manager
Email: ottob [at] who.int (ottob[at]who[dot]int)
Communications and marketing officer
Tel: + 242 06 520 65 65 (WhatsApp)
Email: boakyeagyemangc [at] who.int (boakyeagyemangc[at]who[dot]int)