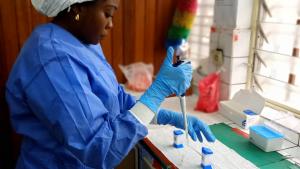
The day the lab techs helped change the fate of a city in the Democratic Republic of the Congo
Medical biologist Espérance Tshiwedi was in a meeting back in July when her phone rang insistently. “What is it?” she snapped to the lab technician on duty. He asked to speak with her in the lab – immediately.
“Instinct told me, something was wrong at the lab,” explains the woman in charge of the Goma laboratory of the National Institute of Biomedical Research. She ran.
“I was scared. At first glance, I did not want to believe it,” she continues, describing the test results the technician showed her. “I stared at those four curves. I quickly asked if we could run the analysis again, and we did. As the second results came in, we confirmed the first Ebola case in Goma.”
Emotions among the many technicians there was overwhelming, she remembers. “Everyone around the room seemed to gasp. This sample came in like any other does on a typical day at the lab. In that instant, there was only one thing to do.”
The lab coordinator alerted the Ministry of Health and the head of the National Institute of Biomedical Research and the many others in the chain of information-sharing that then triggered the swift reaction and ultimately contained the spread of that case.
It was a conclusion no one wanted to see but everyone had been bracing for in the concerted efforts to prepare for the worst in what is now the tenth and longest Ebola outbreak in the Democratic Republic of the Congo (DRC): that the epidemic would spread into Goma, the provincial capital of North Kivu and home to more than a million people.
The health clinic nurse who had suspected the case and Goma local technicians who analysed the sample that the nurse had sent became local heroes for “saving” the city from what easily could have been a terrible situation.
“We are proud of our quick actions as a team. I am grateful for my team for their determination and sacrifice all throughout these past months,” says Tshiwedi.
Surveillance and rapid detection of an Ebola case are proving to be vital tools in the race to end this outbreak, and case numbers have been dwindling for the past several months. To provide quicker lab analysis needed for quick detection, the Government, in collaboration with the World Health Organization and partners, expanded on an approach started in the previous outbreak but with only a single unit. This time, multiple “mobile” laboratories that operate as extensions of the National Institute of Biomedical Research were set up in field locations because closer proximity to outbreak hot spots speeds up the confirmation of a case.
Twelve field labs have been functioning since the first one (in Beni) opened on day 3 of the outbreak, including the Goma laboratory that Tshiwedi manages, which opened on day 12 of the outbreak, which was declared on 1 August 2018. They are in the three affected north-eastern provinces of North Kivu, Ituri and South Kivu (with Beni as a headquarter, Goma, Butembo, Katwa, Mangina, Mambassa, Komanda, Mwenga, Bukavu and Bunia, with two recently opened in Biakato and Kasindi).
Together, they have tested more than 100 000 samples to date. The Goma laboratory has tested more than 5240 samples since opening in mid-August 2018.
The laboratories helped contain the rising number of cases quickly, says Dr Daniel Mukadi, coordinator for the mobile laboratories. “We have benefited from GeneXpert trainings for good laboratory practices, organized by WHO, and also from the United States Center for Disease Control and Prevention (US CDC) trainings on biosecurity, packaging safety and transport of infectious material.”
The proficiency to protect the communities around them is not going anywhere once the Ebola outbreak ends, he says. “We have well-trained staff to ensure the continuity of these activities.” Today, he adds, “the laboratories in these provinces run efficiently and are prepared for any given situation.” The laboratories will stay in place for a year after the end of the outbreak and will include monitoring the health conditions of the people enrolled in the Ebola survivors programme.
“It is a significant achievement for the National Institute of Biomedical Research to have expanded its range of action widely to address challenges posed under Ebola,” Dr Mukadi says. More specifically, they were put in place in a short time frame, he adds.
Along with WHO, other partners, including Médecins Sans Frontières, UNICEF, the US CDC, Ajaka and the Institute of Research in Montpellier (France), worked with the National Institute of Health to establish this network of mobile laboratories.
For the Ministry of Health to have its own network of national laboratories, fully managed by national staff, demonstrates the Government's commitment to improve its surveillance system at the national level, says Dr Mukadi. “The work we have been able to accomplish together is impressive. The feeling in general is of success – we are proud of it.”
With Ebola a highly contagious virus, the initial responders in health clinics and laboratory technicians are vulnerable. But good preparedness and proper procedures have improved their safety. And without doubt, the dedication of the many professionals on the Ebola front line in the DRC has been a major contribution to saving lives.
“It is true that, with the work we do, we have potential to be highly exposed to Ebola. Yet, here in Goma, it has been contained,” says Tshiwedi. “The lab is my profession, and what I do is in my blood. I love the work I do.”
Consultant
Phone: +243 820 66 46 24
Communications and marketing officer
Tel: + 242 06 520 65 65 (WhatsApp)
Email: boakyeagyemangc [at] who.int (boakyeagyemangc[at]who[dot]int)