Key fact

Cervical cancer
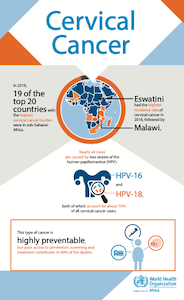
is highly preventable,
but poor access to prevention, screening and treatment contributes to 90% of the deaths.
Featured video
Cervical cancer is a type of cancer that occurs in the cells of the cervix, or lower part of the uterus that connects to the vagina. Nearly all cases are caused by oncogenic strains of human papillomavirus (HPV), specifically two strains, HPV-16 and HPV-18, both of which account for about 70% of all cervical cancer cases. When people are exposed to HPV such as through sexual activity, the virus can be transmitted through skin-to-skin contact and body fluids. Women who are HIV-positive are five times more likely to develop invasive cervical cancer and the progression from precancer to cancer takes a much shorter time.
Although country-specific data are limited, the most recent data from the International Agency for Research indicate that there were 111 632 new cases in 2018 in sub-Saharan Africa. In the same year, 68% of women died from cervical cancer.
Women are at higher risk if they:
- Are HIV-positive or have any other condition that makes it hard for the body to fight off illness
- Have had multiple sexual partners, have sex with partners who themselves have multiple sexual partners, or participate in high-risk sexual activity
- Have not been vaccinated against HPV
- Have a coinfection involving other sexually transmitted agents such as herpes simplex virus 2 (HSV-2), Chlamydia trachomatis and Neisseria gonorrhea
- Smoke; the risk increases according to how much they smoke and the age at which they started smoking
- Have engaged in long-term use of oral contraceptives
- Have not been screened for precancer lesions.
Early stage cervical cancer generally produces no signs or symptoms, but for women who get screened for cervical cancer, an abnormal result showing occurrence of precancerous lesion is usually the first sign of this disease.
Early symptoms that may occur can include:
- Abnormal vaginal bleeding between periods, after intercourse, or after menopause
- Continuous vaginal discharge (pale, watery, pink, brown, bloody or foul-smelling)
- Heavier periods that continue for longer than usual.
Signs and symptoms of progressive cervical cancer include:
- Vaginal bleeding after sex
- Pelvic pain or pain during sex
- Offensive vaginal discharge
- Abnormal bleeding between menstrual periods, heavier periods, or bleeding after menopause
- Increased or painful urination, or urinary infection
- Lower back or leg pain, or a single swollen leg
- Bone fractures
- Unexplained weight loss.