WHO supports Botswana to respond to an outbreak of diarrhoea in children below five years of age
Gaborone, Botswana - 29 October 2018: Botswana has been experiencing an outbreak of diarrhoea mainly affecting children below five years of age since the beginning of September 2018. The diarrhoea outbreak started in the central part of the country and then spread to other districts. At the peak of the outbreak, 18 of the 27 districts in Botswana reached epidemic level. The outbreak was detected through analysis of routine surveillance data. Laboratory investigations attributed the cause of the outbreak to rotavirus. Rotaviruses are recognized as the single most important cause of severe infantile gastroenteritis worldwide. Like many African countries, Botswana introduced rotavirus vaccine (RotarixTM) into the national immunization programme in July 2012.
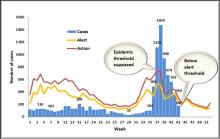
The upsurge in cases of diarrhoea with dehydration among children below five years was observed in week 36 (3 – 9 September 2018). The cases rapidly increased reaching the established national epidemic threshold in week 37 (10 - 16 September 2018) and peaking in week 38 (17 - 23 September 2018) before beginning to decline steadily. Between week 36 (3 - 9 September 2018) and week 42 (15 - 21 October 2018), 5606 cases of diarrhoea with dehydration were reported. During the same period, 37 deaths occurred, giving a case fatality ratio of 0.7%. The direct causes and reasons for these deaths are being investigated by the National Mortality Audit Committee, in line with the country’s policy of “No tolerance to infant mortality”. Additionally, there were 494 cases of diarrhoea with blood and 31,198 cases of diarrhoea without dehydration in children below five years, reported during the same period. Diarrhoea cases were also reported among persons older than five years of age; however, the numbers were relatively small.
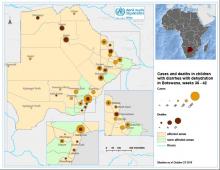
As of week 42, the country has come out of epidemic phase; however, three districts (Gaborone, Kanye and North-east) are still in active epidemic phase, nine districts are in alert phase while 16 districts are below the alert threshold. The districts in the eastern and north-eastern part of the country are most affected, corresponding with urbanization and population density pattern.
Of 228 stool specimens analysed at the National Health Laboratory (NHL) in Gaborone, 152 (67%) were positive for rotavirus using ELISA. Thirty-four (72%) out of 47 specimens analysed at the WHO Regional Reference Laboratory for rotavirus in South Africa identified rotavirus genotype G3P8 as the most common strain during this outbreak. Between 8th and 19th October 2018, the NHL cultured 22 stool specimens and all the specimens were negative for Vibrio cholerae. No suspected cholera cases have been detected in Botswana in recent times.
In response to the diarrhoea outbreak, the Botswana Ministry of Health and Wellness, WHO and the University of Botswana School of Public Health implemented several outbreak control measures, structured under the following thematic areas: coordination and leadership, epidemiology and laboratory, case management, social mobilization/advocacy and communication, water, hygiene and sanitation (WASH), and finance, administration and logistics.
The WHO Country Office in Botswana, the WHO Regional Office for Africa, Brazzaville Congo and the Inter-country Support Team based in Harare, Zimbabwe provided technical assistance to the Ministry of Health and Wellness. Two WHO technical experts worked with the National Rapid Response Teams to conduct detailed outbreak investigations and analysis of the available data in order to gain deeper understanding of the factors responsible for the occurrence of the outbreak. The team also reviewed the ongoing response measures and provided guidance to improve effectiveness of the interventions.
On 26 October 2018, the WHO experts debriefed senior management of the Ministry of Health and Wellness headed by the acting Permanent Secretary, Ms B Moagi, in the presence of the WHO Representative and country team. The acting Permanent Secretary emphasized the need to closely monitor the quality of water, which is usually the main cause of diarrhoea diseases. She also reiterated the importance of multi-sectoral collaboration in addressing health determinants responsible for most communicable diseases, which are usually outside the remit of the health sector. She noted that the Emergency Operations Centre being established will go a long way in improving coordination and response to epidemics in the country.